Research Article
First Long-Term, Eleven-Year, Parasitological Surveys, during a Village-Scale Malaria Vector Control Program in Angola 
2 OCEAC (Organisation of Coordination for Endemic Diseases Control in Central Africa), Yaoundé Cameroon
3 Malaria Control Program, Medical Department, Sonamet, Lobito, Angola
4 Hygiene Safety Environment, Batuan, Bali Indonesia
 Author
Author  Correspondence author
Correspondence author
Journal of Mosquito Research, 2026, Vol. 16, No. 2
Received: 01 Apr., 2026 Accepted: 20 Apr., 2026 Published: 30 Apr., 2026
Objectives
At the request of, and together with the National Malaria Control Program of Angola (NMCPA), a comprehensive program was planned, and implemented, in villages around Balombo town (Benguela Province) with two objectives: to compare, in natural conditions, the efficacy of four methods of vector control; and to check for any parasitological rebound effect several years after vector control.
Patients and Methods
Four vector control methods were implemented: long-lasting deltamethrin treated nets (LLIN), PermaNet®2.0 (P2) alone; P2 combined with deltamethrin insecticide-treated plastic sheeting (ITPS) model ZeroFly®; ITPS model ZeroVector® alone, and two rounds of lambdacyhalothrin indoor residual spraying (IRS) followed by ITPS installation. Each method was implemented in one village. Several analyses of short-term entomological, parasitological, and immunological impact had already been published. The long-term, eleven years, parasitological evaluation was performed in these four villages, and was based upon regular cross-sectional surveys on random samples of volunteer’s asymptomatic children ≤15-year-old. Thick blood films were made in the field, and examined by optical microscope in the medical department of the Angolese Sonamet® Company in Lobito which implemented, and supported, its Malaria Control Program (MCP) in Benguela Province. The Balombo program was a part of this MCP. Three parasitological indicators were analyzed: Plasmodium parasite prevalence, parasite load and gametocyte index.
Results
From the year 2007 to the year 2018, 136 parasitological cross-sectional surveys were performed. 12,525 thick blood films (TBF) were prepared. Plasmodium were observed in 2,392 TBF, i.e., a parasite prevalence of 19.1%, and gametocytes in 247 blood films, i.e., a gametocyte rate of 1.97%. Parasite prevalence (PP) for the two years before vector control (years 2007-2008) (PP=39.4%; n=4,302) and the nine years after (years 2009-2018) (PP=8.5%; n=8,223) showed a significant 78.4% decrease. This decrease was similar with all four methods: -77.8% with treated nets alone; -76.9% with the combination nets + ITPS ZeroFly®; -80.8% with ITPS ZeroVector® alone; and -76.8% with indoor spraying followed by ITPS installation. After vector control there was observed an evolution of the parasite prevalence in three successive steps: first an important drop of 61% the first year following vector control and another 64% the following year. Then, over several years, occurred a plateau, which remained at a low parasite prevalence level (< 5%) until the 2015 national malaria outbreak, which induced an increase of the parasite prevalence. But, even during this time, the parasite prevalence (PP=17.8%; n=991) was still significantly lower than before vector control. The impact of the national malaria outbreak was also clearly observed on the parasite load which increased significantly. The gametocyte index, and the parasite load, had the same “three steps” evolution as parasite prevalence after vector control. The several years of low plasmodial infections were a crucial epidemiological indication. No rebound effect of parasite prevalence was noticed ten years after vector control.
Conclusion
The four methods of vector control similarly reduced Plasmodium prevalence, gametocyte index, and parasite load. Ten years after vector control, the parasite prevalence was still lower than before vector control despite the national malaria outbreak and no rebound was noticed. During the malaria outbreak it was observed a significant increase of the parasite load which could be matter of concern. Actual community participation, observed during ITPS installation inside their homes, was a crucial point for the sustainability, and therefore efficacy, of this vector control method. Therefore, ITPS alone, or in combination with treated-nets, could be recommended, as an additional complementary, tool in the arsenal of the National Malaria Control Program of Angola, and other countries.
1 Introduction
According to a WHO World Malaria Report, malaria is still a major public health concern in Angola (37 million of inhabitants) with 8 251 449 estimated malaria cases and 16 169 estimated deaths in 2023 (World Health Organization, 2024). «The accuracy of malaria prevalence estimates in Angola has traditionally been somewhat compromised by incomplete reporting, inability to test due to stockouts of the necessary materials, and other logistic challenges, such as transportation of materials to remote areas and efficient distribution. » (Plucinski et al., 2017; Programa Nacional de Controle da Malaria, 2019; U.S. President’s Malaria Initiative, 2019; Tavares et al., 2022). The situation is worsening with drugs resistant P. falciparum (Fortes et al., 2011; Ngane et al., 2015; Fançony et al., 2016) and the National Malaria Control Program of Angola (NMCPA) developed a comprehensive program, including intermittent preventive treatment for pregnant women (Fortes, 2011) and the use of ACTs as first line treatment of uncomplicated malaria (Guthmann et al., 2005; Plucinski et al., 2017; Davlantes et al., 2018).
A special accent was given to vector control, but due to the failure of inside residual spraying (Somindjinga et al., 2009), the program has focused on large-scale distributions of insecticide-treated nets. (ITN/LLIN) (U.S. President’s Malaria Initiative, 2020; U.S. President’s Malaria Initiative, 2021). Recent studies showed that one year after distributions the ITN coverage dropped from 98% to 63% (Morais et al., 2019) “indicating that new ITNs/LLINs must be continuously supplied to replace those that have lost efficacy and are torn, in order to maintain high levels of coverage.” (Tavares et al., 2022). But, in Angola, as elsewhere, there is a problem of non-use, or misuse, or re-use of nets (Eisele et al., 2011; McLean et al., 2014; Kibe et al., 2019). Surveys in village around Balombo reported that it two or-three years, most of distributed LLINs were withdrawn (Carnevale et al., 2021), and, simultaneously, parasite prevalence increased. One of the key points for the success of a malaria vector control is its sustainability, which depends, among other things, on actual community participation (Monroe et al., 2021), the tools selected, the insecticide resistance, and the availability resources in the short, middle and long term.
A “malaria disaster” was feared with the spread of pyrethroid resistance (Hemingway and Ranson, 2000; Hemingway et al., 2016; Ranson and Lissenden, 2016), which could contribute to reduced efficacy of insecticide-treated nets (N'Guessan et al., 2007), as could other factors (Kleinschmidt et al., 2015). It was proposed to combine pyrethroid treated long-lasting nets with indoor residual spraying (Kleinschmidt et al., 2009; Protopopoff et al., 2015) with other classes of insecticide, or to combine two different insecticides on the same nets, (Guillet et al., 2001) or to add on (or in) the nets a synergist such as piperonyl (Pennetier et al., 2013; Protopopoff et al., 2018; Martin et al., 2021; Tungu et al., 2021; Mechan et al., 2022; Roh et al., 2022), or juvenile hormone analog such as pyriproxyfen (Djènontin et al., 2015; Sagnon et al., 2015; Tiono et al., 2015; Tiono et al., 2018; Toé et al., 2019), or chlorfenopyr (Ngufor et al., 2011; Accrombessi et al., 2023; Zahouli et al., 2023; Accrombessi et al., 2024; Sovi et al., 2024; Yovogan et al., 2024) and this could increase the price of the net.
According to these difficulties in LLINs, in term of implementation, efficacy and sustainability, it clearly appeared a need for new tools, and the recently developed insecticide-treated plastic sheeting (ITPS) seemed to be an interesting option for malaria control (Burns, 2005; Diabate et al., 2006; Messenger et al., 2012). Treated with pyrethroid they were of great efficacy in refugee camps (Burns, 2005), or combined with LLIN (Chandre et al., 2010) or treated with carbamates and then combined with (Djenontin et al., 2009; Djènontin et al., 2010) or treated with organophosphate (Ngufor et al., 2014).
Therefore, combining treated nets and ITPS (or IRS) seemed to be an interesting approach (Kleinschmidt et al., 2009; Okumu et al., 2013). Considering their reported efficacy, and acceptability (Messenger et al., 2012), ITPS appeared worthy of epidemiological evaluation in villages around Balombo town as the acceptability of ITPS had already been observed in the close town of Huambo (Messenger et al., 2014).
The project was a part of the current Malaria Control Program of the Sonamet® Angolese Company, it was requested by the National Malaria Control Program of Angola, which gave clearance and support; the public health department of the Benguela province was actually involved in field surveys. The project had two objectives: to comprehensively compare the feasibility, and efficacy, of four methods of vector control, each one in one village, in completely natural conditions, without disturbing other measures implemented in the region by National or Non-Governmental Organizations (Brosseau et al., 2012; Carnevale et al., 2024). The second objective was to check for any long-term negative parasitological impact, called “rebound effect”, meaning a sharp increase of plasmodial infections which could occurred several years after vector control, supposed to have decrease immunity.
2 Methods
The ecological and social situations of Balombo area (Benguela Province, Angola) (12° S; 14° E) and the villages studied were already presented (Brosseau et al., 2012; Carnevale et al., 2024) (Figure 1). The villages for the Balombo trial were selected by the National Malaria Control Program of Angola, they far each other to avoid any “contamination” of mosquitoes going from one to another one village and influencing catches samples.
|
Figure 1. Map of the area (Adopted from Brosseau et al., 2012). |
The demographic situation, tools for vector control and the flow diagram of vector control implementation are presented in Table 1.
|
Table 1. Demographic information on the four villages involved, at the beginning of the project in February 2007 (* a sleeping unit was defined as any item used for sleeping, including permanent beds, temporary mats, cardboard, loincloths, and other items unfolded at night to sleep). |
Each one of the four villages of this study received one vector control method only, with complete coverage of each house which were already numbered and geo-localized following classical protocol for planning, implementing and monitoring vector control operations (García et al., 2019). This approach was used to identify house with “at least” one member having a positive thick blood films at each survey and localize eventual “hot spot (Soares Magalhães et al., 2012).
Four tools were used for vector control:
-Long-lasting insecticide-treated nets (LLIN), model “PermaNet® 2.0”, treated at 55 mg a.i. deltamethrin (δ)/m2; with a surface area of 13 m2, the total amount of insecticide was 0.715 gr a.i. deltamethrin/LLIN.
-Insecticide-treated plastic sheeting (ITPS), model “ZeroVector” ® (ZV) treated at 170 mg a.i. δ/m2 and presented in rolls.
-Insecticide-treated plastic sheeting, model “ZeroFly®” (ZF), treated at 360 mg a.i. δ/m2; with a size of 19.11 m2, the total amount of insecticide was 6.88 gr a.i. δ/ ZeroFly®.
-Sachets of lambdacyhalothrin (λ) “Icon® WP”, 6.25 gr a.i. λ/sachet for indoor residual spraying, (IRS) targeting 25 mg a.i./m2 of sprayed surface, two rounds, followed by installation of ITPS.
Full coverage in LLIN, ITPS, and the first round of IRS were achieved in December 2008 (Table 2).
|
Table 2. Vector control operations in the four villages of the trial. C= control village, without any vector control operation implemented; xx = no intervention; LLIN = long-lasting insecticide treated net PermaNet 2.0; ITPS= insecticide-treated plastic sheeting; ZF = ITPS model ZeroFly®; ZV= ITPS model ZeroVector®; IRS= inside residual spraying; m2= covered surface; δ=deltamethrin; ʎ=lambdacyhalothrin). |
In Cahata it was given 530 LLINs P.2.0 for 154 houses and 442 sleeping units assuming a complete coverage. In Capango it was given 93 LLINs P2.0 for 60 houses and 89 sleeping units assuming also a complete coverage. The parasitological follow-up was scheduled to occur for 11 years; the first parasitological survey was done in February 2007 and the last in February 2018. Long-term parasitological study was based on regularly done cross-sectional surveys (CSS) for each survey (Brosseau et al., 2012), to get parasite prevalence on randomly selected volunteer’s asymptomatic children≤15-year-old in the four villages.
Thick blood films (TBF) were done, and colored in the field, then examined with optical microscope in the medical department of the Angolese Sonamet® Company in Lobito, with double-check of 10% of TBF in the parasitological laboratory of OCEAC in Yaoundé. Plasmodium species were determined, and counted, compared to 200 white blood cells (WBC) then estimated for 1 ml of blood (assuming 8 000 WBC/ml of blood).
Three classical indicators were analyzed: Plasmodium prevalence (PP), parasite load (PL) and gametocyte index (GI). For statistical analyses all Plasmodium infections were combined as P. malariae, P. ovale, and P. vivax, were scarcely diagnosed, and often associated with P. falciparum. Results were given to the village health worker, in each village, for action, according to the National Malaria Control Program of Angola (NMCPA).
Percentages were compared with the classical Chi square (χ2), (with a 0.05 threshold value of p for statistical significance). Parasite load distributions were analyzed using the non-parametric Mann-Whitney U-test (with a significance level (α) of 0,05), for comparison of medians. Graphics of parasite load, with median values, were constructed with GraphPad5® software.
3 Results
From year 2007 to year 2018, 136 parasitological cross-sectional surveys (CSS) were done; 12,525 thick blood films (TBF) were prepared. Plasmodium were microscopically observed in 2,392 blood films, i.e., a parasite prevalence of 19.1%, and gametocytes in 247 blood films, i.e., a gametocyte index of 1.97%, i.e. around 10 times less than parasite prevalence.
3.1 Plasmodial infections in Cahata village (with LLIN)
3.1.1 Plasmodium prevalence
35 surveys (CSS) were done; 3,665 thick blood films were prepared. Plasmodium were observed in 880 blood films (parasite prevalence=24.0%) and gametocytes in 100 blood films (gametocyte index=2.73%) (Table 3).
|
Table 3. Yearly evolution of parasite prevalence in asymptomatic children ≤ 15-year-old in Cahata village (TBF= thick blood films, n= number of TBF examined; PP= parasite prevalence; G+= thick blood films with gametocytes; GI= gametocyte index). |
For parasite prevalence a significant decrease of 35% occurred after the first distribution of nets (from 55.2%; n=739 to 35.9%; n=675), then -44% after the full coverage in nets (PP=20.2%; n=534 in year 2009) (Annex 1). The decrease still occurred the following years (Table 3) with a plateau at a low level (≤5%) until the outbreak of 2015 (Figure 2).
|
Figure 2. Year l. Evolution of parasite prevalence in asymptomatic children ≤15-year-old in each village. |
Between the two first years, 2007-2008 (called “before” vector control) with a parasite prevalence of 46% (n=1,414) and the following nine years (2009-2018), called “after” vector control, the decrease of 78% was striking (PP=10.2%; n=2,251). For the three years of the malaria outbreak (2015-2018) the parasite prevalence (PP=21.6%; n=273) was significantly two times lower than at the beginning of the trial.
3.1.2 Plasmodium load
The parasite load (Figure 3):
|
Figure 3. Yearly evolution of parasite load in asymptomatic ≤15-year-old children in Cahata (the statistically significant P values are in italics; --- = median value). |
-Significantly decreased after the first distribution of treated nets (p-value<0.0001 between 2007 and 2008), increased after the second distribution of nets (p value= 0.0036 between 2008 and 2009);
-Significantly decreased after distribution of nets for full coverage (p-value= 0.0216 between 2009 and 2010);
-Remained very low during four years, until 2015 when it significantly increased at the time of the national malaria outbreak (p value= 0.0035) and remained relatively high despite measures implemented by the National Malaria Control Program, and other organizations.
The four years of low parasite load is noteworthy.
3.1.3 Gametocyte index
The gametocyte index (GI), significantly decreased after full distribution of nets, and remained at a low level over four years (Figure 4).
|
Figure 4. Yearly evolution of gametocyte index in asymptomatic children ≤15-year-old in each village. |
In February 2018, i.e., 11 years after the first distribution of nets, the gametocyte index was about two times less than in February 2007, before any intervention (respectively 2.5%; n=79 and 4.7%; n=738); The same twofold decrease as for parasite prevalence. Even during the malaria outbreak period, the gametocyte index (1.83%; n=273) was significantly lower than before vector control, (5.02%; n=1 414) (χ2= 5.41; p-value= 0.020; OR= 0.35 [0.12-0.92]).
The three parasitological indicators (PP; PL; GI) had same general trends, with a sharp and significant, drop after vector control implementation, then a plateau at a low level, during several years; then an increase linked to the national malaria outbreak.
3.2 Plasmodial infections in Capango village (with nets and ITPS « Zero Fly® »)
3.2.1 Plasmodium prevalence
33 surveys were done; 2,388 thick blood films were prepared; Plasmodium were observed in 370 blood films (parasite prevalence=15.5%) and gametocytes in 45 blood films (gametocyte index =1.88%) (Table 4).
|
Table 4. Yearly evolution of parasite prevalence in asymptomatic children ≤ 15-year-old in Capango village (TBF= thick blood films, n= number of TBF examined; PP= parasite prevalence; G+= thick blood films with gametocytes; GI= gametocyte index). |
The yearly evolution of parasite prevalence (Figure 1) showed:
-A significant natural decrease (by 33%) from year 2007 to 2008; for these two years without intervention the overall parasite prevalence was 35.2% (n=650);
-Then a striking drop of 60% in 2009, the first year after implementation of vector control;
-A decrease maintained the following years: -62% in 2010, then -13% in 2011;
-A plateau at a low level (<5%) until 2015, i.e., seven years after vector control implementation;
-A sharp increase in 2016, and the years after, showing an obvious impact of the national malaria outbreak.
But even during this period, the parasite prevalence (PP=22.5%; n=227) was significantly lower than before vector control (PP=35.2%; n=650) (χ2= 12.6; OR= 0.53 [0.37-0.76]) (Annex 2).
Ten years after vector control, no “rebound effect” of the parasite prevalence was observed.
3.2.2 Plasmodium load
The distributions of parasite load from year 2007 to year 2018 are plotted in Figure 5.
|
Figure 5. Yearly evolution of parasite load in asymptomatic ≤15 years-children in Capango (the statistically significant p-values are in italics; --- = median value). |
A significant reduction occurred in 2009, the first year after implementation of the combination of LLINs and ITPS ZeroFly®. Then a curious increase in 2010, followed by a striking reduction over four years, with a low level of parasite load, until 2015. The impact of the national malaria outbreak was striking in 2016 and 2018, with a significant increase in 2018 (higher than in 2007: p-value =0.0005; and in 2008: p-value <0.0001); but the parasite load in 2016 was similar to 2007 (p-value= 0.9465).
3.2.3 Gametocyte index
The impact on gametocyte index of the combination of LLIN and ZeroFly® installed inside every house, was striking (Figure 4), with five years without detecting any gametocytes in thick blood films. In 2018, the gametocyte index decreased while both parasite prevalence and parasite load increased.
It is worth considering the evolution of the gametocyte index (GI) during three successive periods:
-Before vector control: GI=4.46% (n=650);
-After vector control, but before malaria outbreak (GI= 0.93% (n=1,511);
-During malaria outbreak: GI= 0.88% (n=227), i.e., 80% less than before vector control.
This clearly shows the long-term impact of this vector control method on gametocyte index in this village.
The three parasitological indicators had same evolution in three phases: a significant reduction after vector control; then a plateau at low level for several years, followed by an increase due to the national malaria outbreak. The evolution of gametocyte index still lower than before any intervention is noteworthy.
3.3 Plasmodial infections in Barragem village (insecticide-treated plasting sheeting, Zero Vector® only)
3.3.1 Plasmodium prevalence
35 surveys were done, 3 042 thick blood films (TBF) were prepared, Plasmodium were observed in 584 TBF, i.e., a parasite prevalence of 19.2%; gametocytes were observed in 38 TBF, i.e., a gametocyte index of 1.25% (Table 5).
|
Table 5. Yearly evolution of parasite prevalence in asymptomatic children ≤ 15-year-old in Barragem village (TBF= thick blood films, n= number of TBF examined; PP= parasite prevalence; G+= thick blood films with gametocytes; GI= gametocyte index). |
The evolution of parasite prevalence (Figure 1) had the same general trend as in other villages, with:
-A natural and significant drop of 32% the first two years; for this period (“control”) the overall parasite prevalence was 40.8% (n=1,050);
-A significant drop of 59% between 2008 and 2009, i.e. the first year after implementation of vector control, and another significant drop of 63% the second year (2010) (Annex 3);
-A noteworthy five years with a very low level of parasite prevalence of <5%;
-An increase in 2015, then 2016, and 2018 linked to the national malaria outbreak. During these three years the parasite prevalence was 15.3% (n=229), i.e., 62% lower (significantly) than before vector control. For the period after vector control the parasite prevalence was 7.8% (n=1,992), also significantly lower than before intervention (-81%).
In Barragem also, 10 years after vector control based on the installation of only ITPS on the walls of villagers' houses, no “rebound” of the parasite prevalence was observed despite the malaria outbreak.
3.3.2 Plasmodium load
The parasite load (Figure 6):
|
Figure 6. Yearly evolution of parasite load in asymptomatic ≤15-year-old children in Barragem (the statistically significant p values are in italics). |
- Significantly naturally decreased the first two years, from 2007 to 2008 (p-value< 0.0001);
-Was similar in 2008 (before vector control) and 2009 (after vector control) (p-value= 0.2778);
-Was similar between 2009 and 2010 (P-value= 0.1775); and in 2010 and 2011 (p-value= 0.52);
-Was significantly lower in 2012 than in 2011 (p-value =0.041);
-Significantly increased in 2015 compared to 2007 (p-value= 0.0282);
-Then remained at a similar level between 2015 and 2016, (p-value= 0.7418); and between 2016 and 2018, (p-value= 0.3088);
In 2012, i.e., four years after the installation of wall lining, the parasite load was significantly lower than in 2008, before installation (p-value= 0.0036);
Parasite load remained very low even in 2013 and 2014, i.e., six years after vector control, and it significantly increased with the malaria outbreak.
3.3.3 Gametocyte index
For the two years before vector control the overall gametocyte index (GI) was 2.1% (n=1,050). It remained at this level of approximately 2% the first year after implementation of vector control. Then, and for the eight following years; it remained at a very low level (Figure 4). Only one gametocyte carrier was detected among the 871 thick blood films made between 2011 and 2018.
The impact, on parasitological indicators, of the installation of ITPS only on the walls inside every house, was striking, and appeared having had long action.
3.4 Plasmodial infections in Candiero village (two rounds of IRS then ITPS)
3.4.1 Plasmodium prevalence
33 surveys were done, 3 430 thick blood films were prepared, Plasmodium were observed in 558, i.e., parasite prevalence= 16.3%, and gametocytes in 64 blood films, i.e., gametocyte index= 1.86% (Table 6).
|
Table 6. Yearly evolution of parasite prevalence in asymptomatic children ≤ 15-year-old in Candiero village (TBF= thick blood films, n= number of TBF examined; PP= parasite prevalence; G+= thick blood films with gametocytes; GI= gametocyte index). |
The yearly evolution of parasite prevalence (Figure 1) showed:
-A natural, but significant decrease of 32% during the two years before vector control (Annex 4), and for these two years “control” the parasite prevalence was 32.7% (n=1,188);
-A sharp significant decrease of 48% in 2009, the year with implementation of the two rounds of indoor residual spraying (in January then in June);
-A significant 68% decrease in 2010, with installation of insecticide-treated plastic sheeting in January;
-A stabilization of parasite prevalence the following two years (PP= 23.5% in year 2018);
-During the three years of malaria outbreak the parasite prevalence was 11.8% (Annex 4)
In Candiero also, even with the national outbreak of malaria, Plasmodium prevalence did not present any “rebound” many years after vector control implementation.
3.4.2 Plasmodium load
The parasite load was similar during the two “control” years (while the parasite prevalence significantly decreased). The following years, the reducing parasite load with complete vector control implementation was statistically significant (Figure 7). The impact of the national malaria outbreak on the parasite load was clear in 2015, 2016, and 2018, with a significant increase, compared to period before vector control:
|
Figure 7. Yearly evolution of parasite load in asymptomatic ≤15-year-old children in Candiero. (the statistically significant p-values are in italics). |
-Between 2007 and 2016: p-value= 0.025
-Between 2007 and 2018: p-value< 0.0001
-Between 2008 and 2016: p-value= 0.0185
-Between 2008 and 2018: p-value< 0.0001.
It is important to note how information could be different when considering either parasite prevalence or parasite load. The first two years, prevalence decreased but parasite load was the same. During the outbreak period, parasite prevalence was lower than before vector control, while parasite load statistically increased:
-Year 2007 versus year 2018: p-value =0.0010 (significant difference)
-Year 2008 versus year 2018: p-value < 0.0001 (significant difference)
3.4.3 Gametocyte index
The gametocyte index dropped significantly (by 80.7%) before, and after vector control, from 3.95% (n=1,188) to 0.76% (n= 2,242) (χ2= 43.4; OR=0.18 [0.11-0.32]) and it remained undetectable (with the size of the sample) for five years (Figure 4) before the important increase in 2018 due to the national malaria outbreak.
The key point is this very low level of human infectivity for vectors for several years.
The different evolution of parasite prevalence and parasite load must be noticed.
3.5 Synthesis
In term of parasite prevalence, the four methods of vector control induced (Table 7):
|
Table 7. Evolution of parasite prevalence, by village, and period of the trial (Before= years 2007-2008; Between = years 2009-2014; Outbreak= years 2015-2018). |
-A similar trend in the long-term evolution of parasite prevalence (Figure 1).
-A significant drop by 78.5% for the nine following years after vector control, (PP= 8.5%; n= 8,223).
-A similar overall decrease: -77.8% with LLINs; -76.9% with the combination of LLIN and ITPS; -80.8% with ITPS alone; -76.8% with the sequence IRS then ITPS.
-A sharp, and significant, decrease the first and second year after implementation of vector control.
-A six-year “plateau” at a very low level (≤5%).
-An increase, from year 2015, due to the national malaria outbreak (Figure 8). But even during this period the parasite prevalence (PP= 17.8%; n=991) was lower than before vector control (PP= 39.4%; n=4,302).
|
Figure 8. Overall evolution of parasite prevalence in asymptomatic children ≤15-year-old before, and after, vector control in the four villages studied. |
The longer lasting impact seemed having been obtained by the combination of LLIN and ZF, and the combination of IRS then ITPS.
Another key result, which must be highlighted, is the fact that, in the natural condition of the project, regardless of events and methods of vector control, no significant rebound effect on the parasite prevalence was noted several years after vector control implementation except the increase due to the national malaria outbreak.
In term of gametocyte index: unlike plasmodic index the evolution of gametocyte was different depending on the vector control method implemented (Table 8).
|
Table 8. Evolution of gametocyte index, by village, and period of the trial. (Before= years 2007-2008; Between = years 2009-2014; Outbreak= years 2015-2018). |
It was observed a peak in Cahata which was not observed in other villages (Figure 4), but the low level of GI spanning several years was clear (Figure 9).
|
Figure 9. Overall evolution of the overall gametocyte index in asymptomatic children ≤15-year-old before (years 2007-2008) and after vector control in the four villages studied. |
Comparing the situation “before” and “after” vector control, the gametocyte index decreased by 74.3% in Cahata; 79.4% in Capango; 61.7% in Barragem; and 80.7% in Candiero, for a significant average reduction of 75.4% (χ2=129; OR=0.23 [0.18-0.31]).
The level of reduction of plasmodial infection (before versus after vector control), on a long-term basis, was similar for parasite prevalence (-78%), and gametocyte index (-76%).
The several years with low parasite load, obtained similarly by each vector control method, is an important epidemiological output of the trial. But the influence of the malaria outbreak on the parasite load, which increased significantly, was clearly observed in the four villages. This confirmed the need for the sustainability of vector control implementation to reduce the actual risk of morbidity link to the intensity of parasite load.
4 Discussion
As was well underlined recently, “progress in the fight against malaria has stalled in recent years, highlighting the importance of new interventions and tailored approaches. A critical factor that must be considered across contexts and interventions is human behavior” (Monroe et al., 2021). Several “factors such as acceptance of insecticide-treated nets (ITNs) and indoor residual spraying (IRS), ability and willingness to consistently use and appropriately care for ITNs and refraining from post-spray wall modifications can all impact the success of core vector control interventions.”
Sustainability, one of the keys to the success of malaria vector control, starts with the acceptability of the measures by population. This point was well studied in the area of Huambo, a town close to Balombo, and elsewhere, to gauge the acceptability of ITPS (Messenger et al., 2012; Messenger et al., 2012; Messenger et al., 2014).
“Integrated Vector Management (IVM) suggests making use of the full range of vector control tools available and “the research needed to improve the quality and delivery of mosquito vector control should focus on (among other) the development of effective and eco-friendly tools to reduce the burden or locally eliminate malaria and other mosquito-borne diseases.” (Benelli and Beier, 2017).
The current mass distribution of LLINs is not sufficient and may not be sustainable. We also need to look to the future, beyond LLINs, for tools.” (Macdonald, 2018). Insecticide-treated plastic sheeting (ITPS) could be considered among “future prospects for control of malaria and other vector-borne diseases.” (Messenger et al., 2012). The problems of indoor residual spraying in Angola, (Somindjinga et al., 2009), and the withdrawal of nets observed in villages around Balombo, where more than 50% of nets were torn and discarded within three years, (Carnevale et al. 2021) showed the need for new tools, among which could be insecticide-treated plastic sheeting.
The comprehensive, long-term, village-scale malaria control program implemented around Balombo town compared the efficacy of insecticide-treated plastic sheeting (ITPS) versus classical LLIN or IRS, alone or in combination (Carnevale et al., 2024).
After implementation of vector control the densities of main vectors per CDC Light Trap, installed inside houses, dropped by 72%, infectivity dropped from 4.53%, (n= 375), to 2.73% (n=183), a noteworthy, if not significant, 43% reduction. The entomological inoculation rates (EIR) decreased similarly by 84%. The four methods had same entomological efficacy (Carnevale et al., 2024).
After implementation of vector control the parasite prevalence dropped by 78%, the gametocyte index dropped by 76% and the parasite load decreased significantly; an interesting epidemiological output as parasite load is related to malaria morbidity (Rogier et al., 1996; Bouvier et al., 1997; Rogier et al., 2001). With the four methods it was observed an evolution of parasitological indicators in three steps: first a striking decrease, then a six-year “plateau”, at a low level, then an important increase due to the national malaria outbreak.
During this outbreak, the parasite prevalence was still lower than before vector control but the parasite loads increased. This underlines the awareness needed when analysis a vector control and the choice of indicators before final statement.
A long period without detectable gametocyte (with the technology used) occurred after vector control. Even if it is known that “a sub-microscopic gametocyte reservoir can sustain malaria transmission” (Karl et al., 2011) the “low-level gametocytemia corresponds to reduced likelihood of mosquito infection.”
The combination of LLIN and ITPS greatly increased the amount of insecticide in the house (Carnevale et al., 2024) but it did not seem having produced a particular parasitological advantage compared to LLIN or ITPS alone. This has to be taken into consideration when planning a vector control programme and the need for regular monitoring. Actually, it was reported that the significant increase in insecticide-based malaria vector control in the past decade has resulted in increasing resistance among malaria vectors and this could lead to great operational problems. The management of insecticide resistance is of great concern (Hemingway and Ranson, 2000; World Health Organization Global Malaria Programme, 2012; Hemingway et al., 2016; Ranson and Lissenden, 2016).
Two main types of mechanism have been identified to be involved in insecticide resistance: target-site resistance, due to mutations in the target proteins of insecticides, and metabolic resistance, due to increased detoxification of insecticides (Hemingway and Ranson, 2000). One well-known target site is the knockdown resistance (kdr) caused by mutations in the voltage-gated sodium channel gene, which compromises the binding with pyrethroid insecticides (Martinez-Torres et al., 1998).
A survey was done in 2001, in four sites in the semi-arid coastal provinces of Luanda and Benguela, and two sites in Huambo province to determine the Anopheles species present, their sporozoite rates and the frequency of a kdr allele. It was reported that « of 218 An. gambiae (195 M-form and 23 S-form) genotyped for the West African kdr-resistance allele, all were homozygous susceptible » (Cuamba et al., 2006).
A study was conducted in 2022 at two sentinel sites in the province of Benguela (Alves et al., 2024). It reported « Kdr mutations were surveyed in An. gambiae s.l. The kdr-West L1014F kdr mutation was discovered in both resistant and susceptible An. coluzzii mosquitoes, while the kdr-East L1014S mutation was detected in An. gambiae s.s. for the first time in Benguela Province. No kdr mutations were found in An. arabiensis. An. gambiae s.s. predominantly exhibited the mutant allele L1014F with an allele frequency of 0.90. In total, across both sentinel sites, the overall frequency of 1014F mutation was 0.65, while the 1014S mutation was found to be 0.01. Our study’s novel discovery of the West African kdr-resistance allele 1014F in An. coluzzii and An. gambiae s.s. confirms the presence of pyrethroid resistance in these populations. Interestingly, the first detection to our knowledge of the East African kdr-resistance allele 1014S in An. gambiae s.s. highlights the emergence of this mutation in Benguela Province. This shows the importance of regular monitoring of insecticide resistances in Anopheles gambiae s.s. populations. This finding suggests an emerging challenge in insecticide resistance, previously unrecorded in this region. The detection of mutations involved in pyrethroid resistance was limited to L1014F and L1014S in An. gambiae s.l. Other potential mechanisms of insecticide resistance, such as metabolic resistance, were not yet explored in Angola. »
It is feared that insecticide resistance could negatively impact the efficacy of pyrethroid treated insecticide-treated nets (N'Guessan et al., 2007). But the conclusion could be different according to the method of evaluation, laboratory, experimental huts (Darriet et al., 1999; Asidi et al., 2004; Koffi et al., 2015) or field trial (Rehman et al., 2013). Conclusions could also be different according to the indicators selected: entomological, immunological, parasitological, epidemiological.
In Kafiné village (Côte d’Ivoire), where An. gambiae has a high kdr based resistance to pyrethroids (80%), permethrin treated nets conferred personal protection with reduction of parasitological indicators (Henry et al., 1999) while no entomological impact was noticed (Doannio et al., 1999).
In the Department of Korhogo, (Northern Côte d’Ivoire) a longitudinal study was conducted to evaluate the entomological and epidemiological impact of nets treated with lambda-cyhalothrin in a region with intense transmission due to An. gambiae highly resistant to pyrethroids with a kdr allelic frequency of around 90% (Henry et al., 2005).
After installation of ITN it was observed a reduction of the inoculation rate two times more than what naturally reduction which occurred in villages without nets (relative reduction of 52.8%); and the rate of asymptomatic infections was higher in the untreated group than the treated one: 68.5% versus 56.6%, (p < 0.001). The parasite load was also significantly higher in the untreated group». In the ITN villages, the incidence of clinical malaria attacks per child per year was significantly lower than in the control villages: 0.8 versus 1.8 (p < 0.001). It was concluded that the protective efficacy of treated nets was 56% (95% CI, 25-75%), comparable to the impact of treated nets on susceptible An. gambiae population.
A WHO coordinated great survey was recently implemented (2012-2016) in Benin, Cameroon, India, Kenya, and Sudan, to investigate whether insecticide resistance was associated with loss of effectiveness of long-lasting insecticidal nets and increased malaria disease burden. Pyrethroid long-lasting insecticidal nets were the principal form of malaria vector control in all study areas. In Sudan this approach was supplemented by indoor residual spraying. Cohorts of children from randomly selected households in each cluster were recruited and followed up to measure incidence of clinical malaria and prevalence of infection. Long-lasting insecticidal net users had lower infection prevalence (adjusted odds ratio [OR] 0.63, 95% CI 0.51-0.78) and disease incidence (adjusted rate ratio [RR] 0.62, 0.41-0.94) than did non-users across a range of resistance levels. We found no evidence of an association between insecticide resistance and infection prevalence (adjusted OR 0.86, 0.70-1.06) or incidence (adjusted RR 0.89, 0.72-1.10) « However, in some locations malaria incidence remained high despite high use of nets, emphasising the need for new tools and approaches for malaria prevention if targets for the reduction of the global malaria burden are to be achieved, and to forestall a potential rebound of malaria due to higher resistance in the future » (Kleinschmidt et al., 2018).
Insecticide-treated plastic sheeting (ITPS) may be one of the new tools. It could contribute to solving the key issue of sustainability, with the added benefit of a long-term efficacy that was clearly demonstrated in natural field conditions in this Balombo study. One of the key observations was that insecticide-treated plastic sheeting alone was as efficient as nets, or the combination nets plus ITPS, or IRS. ITPS had also the great advantage of having been well accepted by villagers who installed them in their houses unlike inside sprayings which are done by outsiders.
The result of the Balombo program was in the line of the position of Messenger and Rowland (Messenger and Rowland, 2017) who considered that “while long-lasting insecticidal nets (LLINs) and indoor residual spraying (IRS) are the cornerstones of malaria vector control throughout sub-Saharan Africa, there is an urgent need for the development of novel insecticide delivery mechanisms to sustain and consolidate gains in disease reduction and to transition towards malaria elimination and eradication. Insecticide-treated durable wall lining (ITWL) may represent a new paradigm for malaria control as a potential complementary or alternate longer-lasting intervention to IRS.”
The aim of our study was to compare the efficacy of four methods in close villages and it appeared that insecticide-treated plastic sheeting had similar parasitological efficacy as classic methods (long-lasting insecticide treated nets or inside residual spraying) with two advantages in term of actual long-lasting activity and acceptability by communities.
A key information obtained by this long-lasting survey was that no “rebound effect” was ever noticed whatever the method of vector control was.
5 Conclusion
Seven important information were obtained after these 11 years of regular field studies, 136 parasitological cross-sectional surveys, 12,525 thick blood films done on asymptomatic children ≤15-year-old, and microscopically observed.
The four methods of vector control produced similar results in reducing significantly, and on a long-term basis, parasite prevalence, parasite load and gametocyte index.
After a striking decrease the first year’s post vector control, there was a five to six-year plateau, at a very low level, in the three parasitological indicators.
During the malaria outbreak, parasite prevalence increased but was still significantly lower than before vector control.
No parasite prevalence rebound was ever noticed, in these field natural conditions, several years after vector control. Malaria outbreak induced an increase of the parasite load, underlining the needs for continuous vector control operations.
Insecticide-treated plastic sheeting may represent an interesting substitute, or complement, to classical LLIN and IRS. They could be combined with nets, or house spraying, treated with different insecticides to address the burning issue of insecticide resistance management.
The actual community participation in the ITPS installation in their house must be underlined.
Adding epidemiological efficacy with communities’ participation, ITPS could be one of the most interesting new available, and operational, tools to facilitate the targeted elimination of malaria.
Acknowledgements
We thank the Sonamet® Angolese Company Manager and its Medical Department for their permanent support, and the International Sub Sea 7® Company for its important financial support, which made it possible to carry out these studies.
We thank the different B2B MD in charge of this medical service during our study.
We thank the Ministry of Health and the Dr Fortes Chief of the National Malaria Control Program of Angola for his involvement and monitoring of the study.
We thank the Provincial Public Health Department for their appreciated help in field studies and all administrative issues. Many thanks to agents of MCP: Luis, Almeida, Alcides, who participated in field surveys, and blood films examination.
Many thanks to teacher John for his careful check of the final version with the English editing.
We thank Mr Timelman who procured the material (treated nets, plastic sheeting) for vector control.
Many thanks also to the communities of the villages who were actually involved in different vector control activities.
Many thanks to teacher John for his English editing.
Funding
The Balombo project was supported by the Sonamet® Angolese Company in the framework of its “Malaria Control Program” managed by its Medical Service; and by the International SubSea 7® Company.
Author’s Contributions
PC designed the protocol, participated to field surveys, analyzed data and wrote the manuscript; JCT participated in field surveys, V. F did the training of microscopists, participated in field surveys, thick blood films examination, and double check with feedback. FM was the head of the Medical Department of the Sonamet Company (Lobito) where all slides were observed and checked; GC was involved in the writing and English version.
Declaration of competing interest
The authors declare that they have no competing interest.
Ethics Statement
«This study was conducted in accordance with the Edinburgh revision of the Helsinki Declaration and was approved by the National Malaria Control Program of the Ministry of Health of Angola, the Ethical authority in charge of approving studies on malaria research in Angola. Written consent (signed by the head of each household) was obtained for all individuals enrolled in the study by the SONAMET® Company - Malaria Control Program (MCP) which is responsible for malaria surveillance and control amongst company employees and their families.» (Brosseau et al., 2012). The study was done as part, and with, the National Malaria Control Program of Angola, the Benguela Public Health Provincial Delegation and a part of the, in process, Malaria Control Program of the Angolese Sonamet® Company.
Accrombessi M., Cook J., Dangbenon E., Yovogan B., Akpovi H., Sovi A., Adoha C., Assongba L., Sidick A., Akinro B., Ossè R., Tokponnon F., Aïkpon R., Ogouyemi-Hounto A., Padonou G.G., Kleinschmidt I., Messenger L.A., Rowland M., Ngufor C., Protopopoff N., and Akogbeto M.C., 2023, Efficacy of pyriproxyfen-pyrethroid long-lasting insecticidal nets (LLINs) and chlorfenapyr-pyrethroid LLINs compared with pyrethroid-only LLINs for malaria control in Benin: a cluster-randomised, superiority trial. The Lancet, 401(10375): 435-446.
https://doi.org/10.1016/S0140-6736(22)02319-4
Accrombessi M., Cook J., Dangbenon E., Yovogan B., Sovi A., Adoha C.J., Djènontin A., N'Guessan R., Rowland M., and Protopopoff N., 2024, Effectiveness of pyriproxyfen-pyrethroid and chlorfenapyr-pyrethroid long-lasting insecticidal nets (LLINs) compared with pyrethroid-only LLINs for malaria control in the third-year post-distribution: a secondary analysis of a cluster-randomised controlled trial in Benin. The Lancet Infectious Diseases, 24(6): 619-628.
https://doi.org/10.1016/S1473-3099(24)00002-1
Alves G., Troco A.D., Seixas G., Pabst R., Francisco A., Pedro C., Garcia L., Martins J.F., and Lopes S., 2024, Molecular and entomological surveillance of malaria vectors in urban and rural communities of Benguela Province, Angola. Parasites & Vectors, 17(1): 112.
https://doi.org/10.1186/s13071-024-06214-8
Asidi A.N., N'Guessan R., Hutchinson R.A., Traoré-Lamizana M., Carnevale P., and Curtis C.F., 2004, Experimental hut comparisons of nets treated with carbamate or pyrethroid insecticides, washed or unwashed, against pyrethroid-resistant mosquitoes. Medical and Veterinary Entomology, 18(2) : 134-140.
https://doi.org/10.1111/j.0269-283X.2004.00485.x
Benelli G., and Beier J.C., 2017, Current vector control challenges in the fight against malaria. Acta Tropica, 174 : 91-96.
https://doi.org/10.1016/j.actatropica.2017.06.028
Bouvier P., Rougemont A., Breslow N., Doumbo O., Delley V., Dicko A., Diakite M., Mauris A., and Robert C.F., 1997, Seasonality and malaria in a West African village: does high parasite density predict fever incidence. American Journal of Epidemiology, 145(9) : 850-857.
https://doi.org/10.1093/oxfordjournals.aje.a009179
Brosseau L., Drame P.M., Besnard P., Toto J.C., Foumane V., Le Mire J., Mouchet F., Remoue F., Allan R., Fortes F., Carnevale P., and Manguin S., 2012, Human antibody response to Anopheles saliva for comparing the efficacy of three malaria vector control methods in Balombo. Angola, PLoS ONE, 7(9) : e44189.
https://doi.org/10.1371/journal.pone.0044189
Burns M., 2005, Evaluating insecticide-treated polyethylene sheeting for malaria control in complex emergencies: an intersectoral approach. Humanitarian Exchange, 3131 :4-16.
Carnevale P., Toto J.C., Foumane V. Carnevale S., and Gay F., 2021, Co-evolution of the presence of long-lasting insecticide treated nets and Plasmodium falciparum Welch, 1897 prevalence in Cahata village (Benguela Province, Angola) during a village- scale long-term of malaria vector control program, Asian Journal of Research in Infectious Diseases. 7(4): 21-32.
https://doi.org/10.9734/ajrid/2021/v7i430223
Carnevale P., Toto J.C., Foumane V., Fortes F., Ingles A., Soyto A., and Dos Santos A., 2024, The Balombo Project (Angola). A long-term village-scale malaria vector control program, comparing four methods: long-lasting insecticide-treated nets alone, insecticide-treated plastic sheeting alone or combined with long-lasting insecticide-treated nets, or following two rounds of indoor residual spraying. I. First entomological and parasitological evaluation, Clinical Reviews and Case Reports, 3(6) : 86.
https://doi.org/10.31579/2835-7957/086
Chandre F., Dabire R.K., Hougard J.M., Djogbenou L.S., Irish S.R., Rowland M., and N'Guessan R., 2010, Field efficacy of pyrethroid treated plastic sheeting (durable lining) in combination with long lasting insecticidal nets against malaria vectors. Parasites & Vectors, 3(1): 65.
https://doi.org/10.1186/1756-3305-3-65
Cuamba N., Morgan J.C., Irving H., Steven A., Wondji C.S., and Townson H., 2006, Malaria vectors in Angola: distribution of species and molecular forms of the Anopheles gambiae complex, their pyrethroid insecticide knockdown resistance (kdr) status and Plasmodium falciparum sporozoite rates. Malaria Journal, 5(1): 1-6.
https://doi.org/10.1186/1475-2875-5-2
Darriet F., Guillet P., N'Guessan R., Doannio J.M.C., Koffi A., and Chandre F., 1999, The impact of permethrin and deltamethrin resistance in Anopheles gambiae s.s. on the efficacy of insecticide-treated mosquito nets. World Health Organization Document WHO/VBC/99.1002 and WHO/MAL/99.1088.
Davlantes E., Dimbu P.R., Ferreira C.M., Afonso P., Martins J., Fortes F., Udhayakumar V., Aidoo M., and Plucinski M.M., 2018, Efficacy and safety of artemether-lumefantrine, artesunate-amodiaquine, and dihydroartemisinin-piperaquine for the treatment of uncomplicated Plasmodium falciparum malaria in three provinces in Angola, 2017. Malaria Journal, 17(1): 144.
https://doi.org/10.1186/s12936-018-2290-9
Diabate A., Chandre F., Rowland M., N'Guessan R., Duchon S., Dabire R., and Hougard J.M., 2006, The indoor use of plastic sheeting pre-impregnated with insecticide for control of malaria vectors. Tropical Medicine & International Health, 11(5): 597-603.
https://doi.org/10.1111/j.1365-3156.2006.01605.x
Djènontin A., Ahoua Alou L.P., Koffi A., Zogo B., Duarte E., N'Guessan R., Moiroux N., and Pennetier C., 2015, Insecticidal and sterilizing effect of Olyset Duo®, a permethrin and pyriproxyfen mixture net against pyrethroid-susceptible and -resistant strains of Anopheles gambiae s.s.: a release-recapture assay in experimental huts. Parasite, 22: 27.
https://doi.org/10.1051/parasite/2015027
Djènontin A., Chabi J., Baldet T., Irish S., Pennetier C., Hougard J.M., Corbel V., Akogbéto M., and Chandre F., 2009, Managing insecticide resistance in malaria vectors by combining carbamate-treated plastic wall sheeting and pyrethroid-treated bed nets. Malaria Journal, 8(1): 233.
https://doi.org/10.1186/1475-2875-8-233
Djènontin A., Chandre F., Dabiré R.K., Chabi J., N'Guessan R., Baldet T., and Corbel V., 2010, Indoor use of plastic sheeting impregnated with carbamate combined with long-lasting insecticidal mosquito nets for the control of pyrethroid-resistant malaria vectors. American Journal of Tropical Medicine and Hygiene, 83(2) : 266-270.
https://doi.org/10.4269/ajtmh.2010.10-0012
Eisele T.P., Thwing J., and Keating J., 2011, Claims about the misuse of insecticide-treated mosquito nets: are thrse evidence-based? PLoS Medicine, 8(4): e1001019.
https://doi.org/10.1371/journal.pmed.1001019
Fançony C., Brito M., and Gil J.P., 2016, Plasmodium falciparum drug resistance in Angola. Malaria Journal, 15(1) : 74.
https://doi.org/10.1186/s12936-016-1122-z
Fortes F., 2011, Perfil epidemiológico das principais doenças parasitárias endémicas em Angola, Doctoral Thesis, Universidade NOVA de Lisboa, Instituto de Higiene e Medicina Tropical.
Fortes F., Dimbu R., Figueiredo P., Neto Z., do Rosário V.E., and Lopes D., 2011, Evaluation of prevalences of pfdhfr and pfdhps mutations in Angola. Malaria Journal, 10(1): 22
https://doi.org/10.1186/1475-2875-10-22
García G.A., Hergott D.E.B., Phiri W.P., Perry M., Smith J., Osa Osa Nfumu J., Nzamio J., Fuseini G., Stabler T., Riloha Rivas M., Kleinschmidt I., Schwabe C., and Guerra C.A., 2019, Mapping and enumerating houses and households to support malaria control interventions on Bioko Island. Malaria Journal, 18(1): 283.
https://doi.org/10.1186/s12936-019-2920-x
Guillet P., N'Guessan R., Darriet F., Traore-Lamizana M., Chandre F., and Carnevale P., 2001, Combined pyrethroid and carbamate 'two-in-one' treated mosquito nets: field efficacy against pyrethroid-resistant Anopheles gambiae and Culex quinquefasciatus. Medical and Veterinary Entomology, 15(1): 105-112.
https://doi.org/10.1046/j.1365-2915.2001.00288.x
Guthmann J.P., Ampuero J., Fortes F., Van Overmeir C., Gaboulaud V., Tobback S., Dunand J., Saraiva N., Gillet P., Franco J., Denoncin A., Van Herp M., Balkan S., Dujardin J.C., D'Alessandro U., and Legros D., 2005, Antimalarial efficacy of chloroquine, amodiaquine, sulfadoxine-pyrimethamine, and the combinations of amodiaquine + artesunate and sulfadoxine-pyrimethamine + artesunate in Huambo and Bié provinces, central Angola. Transactions of the Royal Society of Tropical Medicine and Hygiene, 99(7): 485-492.
https://doi.org/10.1016/j.trstmh.2004.11.010
Hemingway J., and Ranson H., 2000, Insecticide resistance in insect vectors of human disease. Annual Review of Entomology, 45(1) : 371-391.
https://doi.org/10.1146/annurev.ento.45.1.371
Hemingway J., Ranson H., Magill A., Kolaczinski J., Fornadel C., Gimnig J., Coetzee M., Simard F., Roch D.K., Hinzoumbe C.K., Pickett J., Schellenberg D., Gething P., Hoppé M., and Hamon N., 2016. Averting a malaria disaster: will insecticide resistance derail malaria control ? The Lancet, 387(10029) : 1785-1788.
https://doi.org/10.1016/S0140-6736(15)00417-1
Henry M, Assi S, Rogier C, Dossou-Yovo J, Chandre F., Guillet P, and Carnevale P. 2005, Protective efficacy of lambda-cyhalothrin treated nets in Anopheles gambiae pyrethroid resistance areas of Côte d'Ivoire. American Journal of Tropical Medicine and Hygiene, 73(5): 859-864.
https://doi.org/10.4269/ajtmh.2005.73.859
Henry M.C., Doannio J.M.C., Darriet F., Chandre F., Guillet P., and Carnevale P., 1999, Efficacité des moustiquaires pré-imprégnées de perméthrine Olyset Net® en zone de résistance des vecteurs aux pyréthrinoïdes. II. Evaluation parasito-clinique. Médecine Tropicale, 59(4): 355-357.
Karl S., Gurarie D., Zimmerman P.A., King C.H., St. Pierre T.G., and Davis T.M.E., 2011, A sub-microscopic gametocyte reservoir can sustain malaria transmission. PLoS One, 6(6) : e20805.
https://doi.org/10.1371/journal.pone.0020805
Kibe L.W., Kamau A.W., Gachigi J.K., Habluetzel A., and Mbogo C.M., 2019, A formative study of disposal and re-use of old mosquito nets by communities in Malindi, Kenya. Malaria World Journal, 6: 9.
Kleinschmidt I., Bradley J., Knox T.B., Mnzava A.P., Kafy H.T., Mbogo C., Ismail B.A., Bigoga J.D., Adechoubou A., Raghavendra K., Cook J., Malik E.M., Nkuni Z.J., Macdonald M., Bayoh N., Ochomo E., Fondjo E., Awono-Ambene H.P., Etang J., Akogbeto M., Bhatt R., Kariuki S., Kleinschmidt I., Donnelly M.J., and the Implications of Insecticide Resistance Consortium, 2018, Implications of insecticide resistance for malaria vector control with long-lasting insecticidal nets: a WHO-coordinated, prospective, international, observational cohort study. The Lancet Infectious Diseases, 18(6) : 640-649.
https://doi.org/10.1016/S1473-3099(18)30172-5
Kleinschmidt I., Mnzava A.P., Kafy H.T., Mbogo C., Bashir A.I., Bigoga J., Adechoubou A., Raghavendra K., Knox T.B., Malik E.M., Nkuni Z.J., Bayoh N., Ochomo E., Fondjo E., Kouambeng C., Awono-Ambene H.P., Etang J., Akogbeto M., Bhatt R., Swain D.K., Kinyari T., Njagi K., Muthami L., Subramaniam K., Bradley J., West P., Massougbodji A., Okê-Sopoh M., Hounto A., Elmardi K., Valecha N., Kamau L., Mathenge E., and Donnelly M.J., 2015, Design of a study to determine the impact of insecticide resistance on malaria vector control: a multi-country investigation. Malaria Journal, 14(1) : 282.
https://doi.org/10.1186/s12936-015-0782-4
Kleinschmidt I., Schwabe C., Shiva M., Segura J.L., Sima V., Mabunda S.J.A., and Coleman M., 2009, Combining indoor residual spraying and insecticide-treated net interventions. American Journal of Tropical Medicine and Hygiene, 81(3): 519-524.
https://doi.org/10.4269/ajtmh.2009.81.519
Koffi A.A., Alou L.P.A., Djènontin A., Kabran J.P.K., Dosso Y., Koné A., Moiroux N., and Pennetier C., 2015, Efficacy of Olyset Duo®, a permethrin and pyriproxyfen mixture net against wild pyrethroid-resistant Anopheles gambiae s.s. from Côte d’Ivoire: an experimental hut trial. Parasite, 22: 28.
https://doi.org/10.1051/parasite/2015028
Macdonald M.B., 2018, Long-lasting insecticidal nets for malaria control in Myanmar and Nigeria: lessons from the past, tools for the future. Global Health Science and Practice, 6(2): 237-241.
https://doi.org/10.9745/GHSP-D-18-00158
Martin J.L., Mosha F.W., Lukole E., Rowland M., Todd J., Charlwood J.D., and Protopopoff N., 2021, Personal protection with PBO-pyrethroid synergist-treated nets after 2 years of household use against pyrethroid-resistant Anopheles in Tanzania. Parasites & Vectors, 14(1): 150.
https://doi.org/10.1186/s13071-021-04641-5
Martinez-Torres D., Chandre F., Williamson M.S., Darriet F., Berge J.B., Devonshire A.L., Guillet P., Pasteur N., and Pauron D., 1998, Molecular characterization of pyrethroid knockdown resistance (kdr) in the major malaria vector Anopheles gambiae s.s. Insect Molecular Biology, 7(2): 179-184.
https://doi.org/10.1046/j.1365-2583.1998.72062.x
McLean K.A., Byanaku A., Kubikonse A., Tshowe V., Katensi S., and Lehman A.G., 2014, Fishing with bed-nets on Lake Tanganyika: a randomized survey. Malaria Journal, 13(1): 395.
https://doi.org/10.1186/1475-2875-13-395
Mechan F., Katureebe A., Tuhaise V., Mugote M., Oruni A., Onyige I., Bumali K., Thornton J., Maxwell K., Kyohere M., Kamya M.R., Mutungi P., Kigozi S.P., Yeka A., Opigo J., Maiteki-Sebuguzi C., Gonahasa S., Hemingway J., Dorsey G., Reimer L.J., and Lynd A., 2022, LLIN evaluation in Uganda project (LLINEUP): the fabric integrity, chemical content and bioefficacy of long-lasting insecticidal nets treated with and without piperonyl butoxide across two years of operational use in Uganda. Current Research in Parasitology & Vector-Borne Diseases, 2 : 100092.
https://doi.org/10.1016/j.crpvbd.2022.100092
Messenger L.A., and Rowland M., 2017, Insecticide-treated durable wall lining (ITWL) : futurs prospects for control of malaria and other vector-borne diseases, Malaria Journal, 16(1) : 213.
https://doi.org/10.1186/s12936-017-1867-z
Messenger L.A., Larsen M., Thomas J., and Rowland M., 2014, Installation of insecticide-treated durable wall lining: evaluation of attachment materials and product durability under field conditions. Parasites & Vectors, 7(1): 508.
https://doi.org/10.1186/PREACCEPT-1577225326135355
Messenger L.A., Matias A., Manana A.N., Stiles-Ocran J., Knowles S., Boakye D., Coulibaly M., and Rowland M., 2012, Multicentre studies of insecticide-treated durable wall-lining in Africa and South-East Asia: entomological efficacy and household acceptability during one year of field use. Malaria Journal, 11(1): 358.
https://doi.org/10.1186/1475-2875-11-358
Messenger L.A., Miller N.P., Adeogun A.O., Awolola T.S., and Rowland M., 2012, The development of insecticide-treated durable wall-lining for malaria control: insights from rural and urban populations in Angola and Nigeria. Malaria Journal, 11(1): 332.
https://doi.org/10.1186/1475-2875-11-332
Monroe A., Moore S., Olapeju B., Merritt A., and Okumu F., 2021, Unlocking the human factor to increase effectiveness and sustainability of malaria vector control. Malaria Journal, 20(1) : 404.
https://doi.org/10.1186/s12936-021-03943-4
Morais J., Francisco M., de Vasconcelos J.N., Tchimbinda A., António F., Martins J., Fortes F., and Arez A.P., 2019, Epidemiological baseline cross-sectional study to monitor Plasmodium falciparum transmission intensity in Southern Angola. Instituto Nacional de Investigação em Saúde (INIS), Centro de Investigação em Saúde de Angola (CISA), Angolan NMCP, Elimination 8, UCSF, Global Fund, Luanda: 49.
Ngane V.F., Djaman J.A., Culeux C., Piette N., Carnevale P., Besnard P., Fortes F., Basco L.K., and Tahar R., 2015, Molecular epidemiology of drug-resistant Plasmodium falciparum in Benguela province. Angola, Malaria Journal, 14(1): 113.
https://doi.org/10.1186/s12936-015-0634-2
N'Guessan R., Corbel V., Akogbeto M., and Rowland M., 2007, Reduced efficacy of insecticide-treated nets and indoor residual spraying for malaria control in pyrethroid resistance area, Benin. Emerging Infectious Diseases, 13(2): 199-206.
https://doi.org/10.3201/eid1302.060631
Ngufor C., Chouaïbou M., Tchicaya E.S., Koffi A.A., N'Guessan R., and Rowland M., 2014, Combining organophosphate-treated wall linings and long-lasting insecticidal nets fails to provide additional control over long-lasting insecticidal nets alone against multiple insecticide-resistant Anopheles gambiae in Côte d’Ivoire: an experimental hut trial. Malaria Journal, 13(1): 396.
https://doi.org/10.1186/1475-2875-13-396
Ngufor C., Fongnikin A., Rowland M., N'Guessan R., Odjo A., Malone D., Vigninou E., Akinro B., Fagbohoun J., Sovi A., Padonou G.G., and Akogbeto M., 2023, Small-scale field evaluation of PermaNet® Dual (a long-lasting net coated with a mixture of chlorfenapyr and deltamethrin) against pyrethroid-resistant Anopheles gambiae mosquitoes from Tiassalé, Côte d'Ivoire. Malaria Journal, 22(1): 36.
https://doi.org/10.1186/s12936-023-04455-z
Ngufor C., N'Guessan R., Boko P., Odjo A., Vigninou E., Adoha C., and Rowland M., 2011, Combining indoor residual spraying with chlorfenapyr and long-lasting insecticidal bed nets for improved control of pyrethroid-resistant Anopheles gambiae : an experimental hut trial in Benin. Malaria Journal, 10(1) : 343.
https://doi.org/10.1186/1475-2875-10-343
Okumu F.O., Mbeyela E., Lingamba G., Moore J., Ntamatungiro A.J., Kavishe D.R., Kenward M.G., Turner E., Lorenz L.M., and Moore S.J., 2013, Comparative field evaluation of combinations of long-lasting insecticide treated nets and indoor residual spraying, relative to either method alone, for malaria prevention in an area where the main vector is Anopheles arabiensis. Parasites & Vectors, 6(1): 46.
https://doi.org/10.1186/1756-3305-6-46
Pennetier C., Bouraima A., Chandre F., Piameu M., Etang J., Rossignol M., Sidick A., Zogo B., Moiroux N., and Corbel V., 2013, Efficacy of Olyset® Plus, a new long-lasting insecticidal net incorporating permethrin and piperonyl-butoxide against multi-resistant malaria vectors. PLoS One, 8(10) : e75134.
https://doi.org/10.1371/journal.pone.0075134
Plucinski M.M., Dimbu P.R., Macaia A.P., Ferreira C.M., Samutondo C., Quivinja J., Afonso M., Kiniffo R., Mbounga E., Kelley J.S., Patel D.S., He Y., Talundzic E., Garrett D.O., Halsey E.S., Udhayakumar V., Ringwald P., and Fortes F., 2017, Efficacy of artemether-lumefantrine, artesunate-amodiaquine, and dihydroartemisinin-piperaquine for treatment of uncomplicated Plasmodium falciparum malaria in Angola. Malaria Journal, 16(1): 62.
https://doi.org/10.1186/s12936-017-1712-4
Plucinski M.M., Ferreira M., Ferreira C.M., Afonso P., Fançony C., Lacerda M., and Fortes F., 2017, Evaluating malaria case management at public health facilities in two provinces in Angola. Malaria Journal, 16(1) : 186.
https://doi.org/10.1186/s12936-017-1843-7
Programa Nacional de Controle da Malária (PNCM), 2019, Relatório Anual Descritivo da Malária, Ministério da Saúde de Angola.
Protopopoff N., Mosha J.F., Lukole E., Charlwood J.D., Wright A., Mwalimu C.D., Manjurano A., Mosha F.W., Kisinza W., Kleinschmidt I., and Rowland M., 2018, Effectiveness of a long-lasting piperonyl butoxide-treated insecticidal net and indoor residual spraying interventions, separately and together, against malaria transmitted by pyrethroid-resistant mosquitoes: a cluster randomized controlled, two-by-two factorial design trial,.The Lancet, 391(10130) : 1577-1588.
https://doi.org/10.1016/S0140-6736(18)30427-6
Protopopoff N., Wright A., West P.A., Tigererwa R., Mosha F.W., Kisinza W., Kleinschmidt I., and Rowland M., 2015, Combination of insecticide treated nets and indoor residual spraying in Northern Tanzania provides additional reduction in vector population density and malaria transmission rates compared to insecticide treated nets alone : a randomized control trial. PLoS One, 10(11) : e0142671.
https://doi.org/10.1371/journal.pone.0142671
Ranson H., and Lissenden N., 2016, Insecticide resistance in African anopheles’ mosquitoes: a worsening situation that needs urgent action to maintain malaria control. Trends in Parasitology, 32(3) : 187-196.
https://doi.org/10.1016/j.pt.2015.11.010
Rehman A.M., Mann A.G., Schwabe C., Reddy M.R., Ronca R., Slotman M.A., and Kleinschmidt I., 2013, Five years of malaria control in the continental region, Equatorial Guinea. Malaria Journal, 12(1) : 154.
https://doi.org/10.1186/1475-2875-12-154
Rogier C., Commenges D., and Trape J.F., 1996, Evidence of an age dependent pyrogenic threshold of Plasmodium falciparum parasitaemia in highly endemic populations. American Journal of Tropical Medicine and Hygiene, 54(6) : 613-619.
https://doi.org/10.4269/ajtmh.1996.54.613
Rogier C., Fusai T., Pradines B., and Trape J.F., 2005, Comment évaluer la morbidité attribuable au paludisme en zone d’endémie ? Revue d'Épidémiologie et de Santé Publique, 53(3) : 299-309.
https://doi.org/10.1016/S0398-7620(05)84607-3
Rogier C., Henry M.C., and Spiegel A., 2001, Diagnostic des accès palustres en zone d'endémie : bases théoriques et implications pratiques. Médecine Tropicale, 61(1) : 27-46.
Roh M.E., Oundo B., Dorsey G., Shiboski S., Gosling R., Glymour M.M., Staedke S.G., Bennett A., Sturrock H., and Mpimbaza A., 2022, A quasi-experimental study estimating the impact of long-lasting insecticidal nets with and without piperonyl butoxide on pregnancy outcomes, Malaria Journal, 21(1) : 5.
https://doi.org/10.1186/s12936-021-04034-0
Sagnon N., Pinder M., Tchicaya E.F.S., Tiono A.B., Faragher B., Ranson H., and Lindsay S.W., 2015, To assess whether addition of pyriproxyfen to long-lasting insecticidal mosquito nets increases their durability compared to standard long-lasting insecticidal mosquito nets : study protocol for a randomized controlled trial. Trials, 16(1) : 195.
https://doi.org/10.1186/s13063-015-0700-7
Soares Magalhães R.J., Langa A., Sousa-Figueiredo J.C., Clements A.C.A., and Vaz Nery S., 2012, Finding malaria hot-spots in northern Angola : the role of individual, household and environmental factors within a meso-endemic area. Malaria Journal, 11(1) : 385.
https://doi.org/10.1186/1475-2875-11-385
Somandjinga M., Lluberas M.M., and Jobin W.R., 2009, Difficulties in organizing first indoor spray programme against malaria in Angola under the President's Malaria Initiative. Bulletin of the World Health Organization, 87(11) : 871-874.
https://doi.org/10.2471/BLT.08.052514
Sovi A., Yovogan B., Adoha C.J., Akinro B., Accrombessi M., Dangbénon E., Assongba L., Salako A.S., Padonou G.G., Messenger L.A., Ngufor C., Cook J., Protopopoff N., and Akogbéto M.C., 2024, Efficacy of pyrethroid-pyriproxyfen and pyrethroid-chlorfenapyr nets on entomological indicators of malaria transmission : third year of a randomised controlled trial in Benin. Scientific Reports, 14 : 12958.
https://doi.org/10.1038/s41598-024-63883-2
Tavares W., Morais J., Martins J.F., Scalsky R.J., Stabler T.C., Medeiros M.M., Fortes F.J., Arez A.P., and Silva J.C., 2022, Malaria in Angola : recent progress, challenges and future opportunities using parasite demography studies. Malaria Journal, 21(1) : 396.
https://doi.org/10.1186/s12936-022-04424-y
Tiono A.B., Ouédraogo A., Ouattara D., Bougouma E.C., Coulibaly S., Diarra A., Faragher B., Guelbeogo M.W., Grisales N., Ouédraogo I.N., Ouédraogo Z.A., Pinder M., Sanon S., Smith T., Vanobberghen F., Sagnon N., Ranson H., and Lindsay S.W., 2018, Efficacy of Olyset Duo® a bednet containing pyriproxyfen and permethrin, versus a permethrin-only net against clinical malaria in an area with highly pyrethroid-resistant vectors in rural Burkina Faso: a cluster-randomized controlled trial. The Lancet, 392(10147): 569-580.
https://doi.org/10.1016/S0140-6736(18)31711-2
Tiono A.B., Pinder M., N'Fale S., Faragher B., Smith T., Silkey M., Ranson H., and Lindsay S.W., 2015, The AvecNet® Trial to assess whether addition of pyriproxyfen, an insect juvenile hormone mimic, to long-lasting insecticidal mosquito nets provides additional protection against clinical malaria over current best practice in an area with pyrethroid-resistant vectors in rural Burkina Faso : study protocol for a randomized controlled trial. Trials, 16(1) : 113.
https://doi.org/10.1186/s13063-015-0606-4
Toé K.H., Mechan F., Tangena J.A., Morris M., Solino J., Tchicaya E.F.S., Traoré A., Mahmoud H., Maas J., Lissenden N., Pinder M., Lindsay S.W., Tiono A.B., Ranson H., and Sagnon N.F., 2019, Assessing the impact of the addition of pyriproxyfen on the durability of permethrin-treated bed nets in Burkina Faso: a compound-randomized controlled trial. Malaria Journal, 18(1): 383.
https://doi.org/10.1186/s12936-019-3018-1
Tungu P., Waweru J., Karthi S., Wangai J., and Kweka E.J., 2021, Field evaluation of Veralin® an alpha-cypermethrin + PBO long-lasting insecticidal net, against natural populations of Anopheles funestus in experimental huts in Muheza, Tanzania. Current Research in Parasitology & Vector-Borne Diseases, 1 : 100030.
https://doi.org/10.1016/j.crpvbd.2021.100030
U.S. President's Malaria Initiative (PMI), 2019, U.S. President's Malaria Initiative Angola Malaria Operational Plan 2020, United States Agency for International Development, Washington DC.
U.S. President's Malaria Initiative (PMI), 2020, U.S. President's Malaria Initiative Angola Malaria Operational Plan FY 2021, United States Agency for International Development, Washington DC.
U.S. President's Malaria Initiative (PMI), 2021, U.S. President's Malaria Initiative Angola Malaria Operational Plan FY 2022, United States Agency for International Development, Washington DC.
World Health Organization Global Malaria Programme, 2012, Global plan for insecticide resistance management in malaria vectors (GPIRM), World Health Organization.
World Health Organization, 2024, World Malaria Report 2024 : Addressing inequity in the global malaria response, World Health Organization, Geneva.
Yovogan B., Sovi A., Djènontin A., Adoha C.J., Accrombessi M., N'Guessan R., and Protopopoff N., 2024, The impact of pyrethroid-pyriproxyfen and pyrethroid-chlorfenapyr long-lasting insecticidal nets on density of primary malaria vectors Anopheles gambiae s.s. and Anopheles coluzzii in Benin : a secondary analysis of a cluster randomized controlled trial. Parasites & Vectors, 17(1) : 7.
https://doi.org/10.1186/s13071-023-06104-5
|
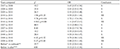
Annex 1 Statistical analysis of the evolution of parasite prevalence in Cahata (S= significant difference; NS= non-significant difference) (before*= years 2007+2008; outbreak**= years 2015+2016+2018; after*** = years 2009 to 2018) |
|
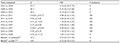
Annex 2 Statistical analysis of the evolution of parasite prevalence in Capango (S= significant difference; NS= non-significant difference) (before* = years 2007-2008; outbreak**= years 2015-2016-2018; after***= years 2009 to 2018) |
|
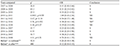
Annex 3 Statistical analysis of the evolution of parasite prevalence in Barragem (S= significant difference; NS= non-significant difference) (before * = years 2007-2008; outbreak **= years 2015-2016-2018; after ***= years 2009 to 2018) |
|
Annex 4 Statistical analysis of the evolution of parasite prevalence in Candiero (S= Significant difference; NS= non-significant difference) (before* = years 2007-2008; outbreak**= years 2015-2016-2018; after ***= years 2009 to 2018) |

. HTML
Associated material
. Readers' comments
Other articles by authors
. Carnevale Pierre
. Toto Jean-Claude
. Foumane Vincent
. Martineaud Franck
. Carnevale Guillaume
Related articles
. Angola
. Vector control at village-scale level with four methods
. Long-lasting insecticide-treated nets
. Insecticide-treated plastic sheeting
. inside residual spraying
. Eleven-year cross sectional parasitological surveys on asymptomatic patients ≤15-year-old
. No parasite prevalence rebound effect
Tools
. Post a comment
.png)
.png)
.png)
.png)
.png)
.png)
.png)
.png)
.png)
.png)
.png)
.png)
.png)
.png)
.png)